
Contact Us

Alzheimer’s disease is a progressive neurological condition that impacts memory, cognition, and daily functioning. It is the most common cause of dementia, affecting millions of people worldwide.
At Neurotherapeutix, we offer fMRI-guided TMS therapy as an advanced, non-invasive treatment that targets key brain regions affected by Alzheimer’s.
If you’re seeking innovative treatment for Alzheimer’s in New York, contact us or continue reading to learn how we can help.
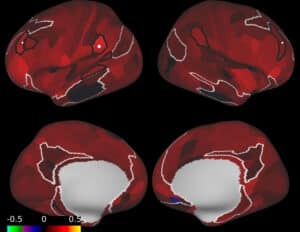
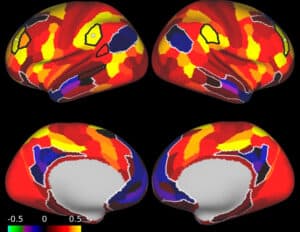
Alzheimer’s disease is a chronic neurodegenerative disorder that gradually impairs memory, language, reasoning, and behavior.
This condition occurs when abnormal proteins accumulate in the brain, disrupting neuron communication and eventually causing cell death.
Alzheimer’s typically affects older adults, though early-onset cases can begin in individuals under 65. As Alzheimer’s progresses through its various stages, patients experience increasing cognitive decline, eventually affecting their ability to maintain independence and perform everyday activities.
There are several forms of Alzheimer’s disease, each with distinct characteristics:
The exact cause of Alzheimer’s disease is not fully understood, but several factors are believed to contribute, including:
Symptoms of Alzheimer’s vary depending on the stage of the disease. Common signs include:
As the disease progresses, individuals may lose the ability to communicate, recognize loved ones, or care for themselves.
Alzheimer’s progresses through several stages:
An Alzheimer’s diagnosis involves multiple steps, which often include:
Early diagnosis allows for more effective symptom management and planning.
Alzheimer’s primarily affects the brain’s default mode network (DMN), the areas responsible for memory, self-awareness, and future planning.
Neurodegeneration in this network leads to:
At Neurotherapeutix, we focus on identifying these specific impairments using advanced functional brain mapping to guide treatment.
Our fMRI-guided TMS therapy offers a new approach to Alzheimer’s care by precisely targeting areas of the brain with weakened connectivity.
This personalized, non-invasive medical service helps restore function by stimulating the brain’s ability to reorganize and form new connections (neuroplasticity).
Key benefits of our approach include:
This methodology improves standard TMS by eliminating the one-size-fits-all model and enabling a data-driven, patient-specific approach.
Alzheimer’s disease begins affecting the brain long before symptoms become apparent.
In fact, structural and functional changes can be detected years before a formal diagnosis. Early intervention is critical for preserving independence, delaying cognitive decline, and improving treatment outcomes.
At Neurotherapeutix, our advanced fMRI-guided approach allows us to:
Intervening during the preclinical or mild cognitive impairment (MCI) stages may significantly slow the progression of Alzheimer’s disease.
While traditional treatments often begin after daily function is already impaired, our technology helps patients take action sooner, when it may make the most significant impact.
If you or a loved one is experiencing early signs of cognitive decline, such as forgetfulness, difficulty focusing, or disorientation, an evaluation at Neurotherapeutix could provide essential insight and support.
Neurotherapeutix is at the forefront of Alzheimer’s treatment in NYC.
Our use of fMRI-guided TMS therapy offers a powerful, non-invasive solution for individuals seeking alternatives beyond traditional medication.
If you or a loved one shows signs of cognitive decline, our personalized therapies may help improve brain function, slow progression, and enhance quality of life.
Please request an appointment or contact us to learn more now.
Call us at (917) 388-3090 or click to request a regular or telehealth appointment.
Neurotherapeutix
171 East 74th Street, Unit 1-1 New York, NY 10021

Neurotherapeutix is the leading clinic for functional imaging guided transcranial magnetic stimulation (TMS), a safe, innovative, and non-invasive methodology for treating a wide range of acute and chronic mental disorders and brain injuries. Our advanced fMRI technology allows us to map the brain for the… Learn More »
By: Neurotherapeutix NYC
Reviewed By: Marta Moreno, Ph.D
Published: March 24, 2023
Last Reviewed: March 5, 2026
QUICK INQUIRY
Contact us to get an estimate for your medical services requirements. You can fill in the form to specify your medical requirements or you can call us directly.