
Contact Us

Living with obsessive-compulsive disorder can be exhausting, especially when intrusive thoughts and repetitive behaviors continue despite medication or therapy.
For many people, OCD affects far more than daily routines. It can interfere with work, relationships, concentration, sleep, and overall quality of life.
If you have tried medication without enough relief, TMS for OCD may offer another path forward.
TMS is an FDA-cleared, non-invasive, outpatient treatment that targets the brain circuits involved in obsessive-compulsive disorder. At Neurotherapeutix, we use functional imaging-guided treatment planning to personalize care based on how your brain networks are functioning.
In this guide, we explain how fMRI-guided TMS works for OCD, who may be a candidate, what to expect during treatment, and how Neurotherapeutix’s precision-based approach helps patients in New York City explore a more targeted treatment option. unique functional guided transcranial magnetic stimulation (TMS). Through brain mapping for TMS, we can specifically target the neural pathways involved in OCD, optimizing treatment outcomes.

Obsessive-compulsive disorder is a chronic neuropsychiatric condition characterized by unwanted, intrusive thoughts, images, or urges called obsessions, along with repetitive behaviors or mental rituals called compulsions.
These compulsions are usually performed to reduce anxiety or prevent something feared from happening, but the relief is often temporary. Over time, the cycle becomes self-reinforcing and more disruptive.
A person with OCD may spend more than an hour each day managing obsessions and compulsions. Symptoms can significantly affect daily functioning, relationships, work, school, and emotional well-being.
OCD is not simply being organized, perfectionistic, or overly worried. It is a medical condition involving distressing thought patterns and repetitive behaviors that can feel difficult or impossible to control.
OCD symptoms vary from person to person, but they often fall into recognizable categories.
Common obsessions may include:
Common compulsions may include:
OCD exists on a spectrum of severity. Some people experience symptoms that are manageable but still distressing, while others find that OCD takes over large portions of the day.
According to the National Library of Medicine, clinicians often use the Yale-Brown Obsessive Compulsive Scale (Y-BOCS) to assess symptom severity and guide treatment planning.
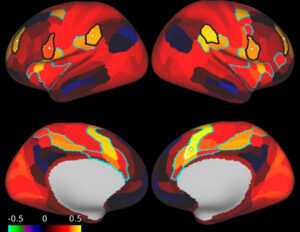
Research increasingly shows that OCD involves dysfunction in specific brain circuits rather than simply a problem with worry or behavior alone. Several regions are thought to play a central role, including the orbitofrontal cortex, anterior cingulate cortex, caudate nucleus, and thalamus.
These brain regions are part of what is often called the cortico-striato-thalamo-cortical, or CSTC, loop. When this loop becomes overactive, the brain may have difficulty shifting away from intrusive thoughts or stopping repetitive urges. That is part of what creates the “stuck” feeling many people with OCD describe.
Understanding OCD at the circuit level reveals why talk therapy and medication alone don’t work for everyone. It also underscores the importance of advanced interventions like fMRI-guided TMS.
By using precise functional imaging to map your unique brain activity and connectivity patterns, we can fully personalize your treatment—delivering pinpoint, targeted stimulation to the neural pathways that need support.
Transcranial magnetic stimulation is a non-invasive treatment that uses magnetic pulses to stimulate targeted areas of the brain.
TMS does not involve surgery, sedation, or seizure induction. Instead, a magnetic coil is placed against the scalp to deliver focused stimulation to specific neural circuits involved in symptoms.
For OCD, TMS is used to help regulate overactive brain pathways associated with obsessions and compulsions. Repeated stimulation can support neuroplasticity, which is the brain’s ability to reorganize and form healthier patterns of activity over time.
Standard TMS and deep TMS are both used in clinical care. Deep TMS is designed to reach deeper brain regions, while standard TMS targets cortical networks closer to the brain’s surface. At Neurotherapeutix, we elevate treatment planning through functional computational brain mapping, moving beyond standard clinical averages. By mapping your unique brain activity and connectivity patterns, we can deeply personalize your care. To ensure maximum precision, we utilize specialized TMS coils designed to deliver targeted stimulation at varying depths—whether superficial or deep—allowing us to successfully reach the exact brain regions driving your OCD symptoms.
TMS received FDA clearance for OCD in 2018, marking an important advancement for people who had not responded adequately to traditional treatment. That clearance was based on clinical research showing meaningful symptom improvement in patients with OCD.
At Neurotherapeutix, we take the proven foundation of FDA-cleared TMS technology and elevate it with functional imaging-guided targeting. By mapping your brain’s unique activity and complex connectivity patterns, we transform standard treatment into a deeply personalized therapy. This ensures your care remains rooted in established, trusted science, while the application itself becomes profoundly more precise, customized, and data-driven.
OCD is associated with overactivity in the brain circuits that regulate fear, error detection, and repetitive thinking. TMS works by delivering magnetic stimulation to brain regions involved in those circuits, helping calm or rebalance the hyperactive loop.
For OCD, treatment often focuses on regions such as the supplementary motor area and medial prefrontal cortex, depending on the protocol and the patient’s individual presentation. At Neurotherapeutix, we use individual fMRI findings to identify unique brain regions involved in OCD, going far beyond the standard targets used in conventional TMS protocols.
Over a series of sessions, repeated stimulation can help reduce the intensity of obsessive thoughts and compulsive urges by promoting healthier communication between connected brain regions.
What makes Neurotherapeutix different is how your treatment is planned.
Our physicians use fMRI-guided TMS therapy, supported by patented computational brain mapping technology, to identify the neural circuits most closely related to your symptoms. Functional MRI allows us to observe how different areas of your brain communicate in real time, helping our team understand where dysregulation may be occurring.
This information guides how TMS stimulation is delivered. Instead of relying only on standard anatomical landmarks used in traditional TMS protocols, fMRI-guided TMS therapy uses your brain’s unique activity and connectivity patterns to personalize and pinpoint your treatment targets with millimeter-level precision and unmatched specificity.
Because every brain functions differently, OCD symptoms can vary widely between individuals. One person may struggle primarily with contamination fears and repetitive checking, while another may experience intrusive thoughts or mental rituals.
By combining TMS with fMRI-based computational brain mapping, Neurotherapeutix can align stimulation with the neural networks associated with your specific symptoms.
This precision-driven approach reflects Neurotherapeutix’s mission to combine advanced neuroscience with compassionate care, helping support healthier brain function and improved quality of life.
TMS may be a good fit for adults with moderate to severe OCD who have not improved enough with traditional treatment. Many candidates have already tried one or more selective serotonin reuptake inhibitors, or SSRIs, without adequate relief.
Others may have stopped medication because of side effects such as fatigue, weight gain, gastrointestinal symptoms, or sexual dysfunction.
TMS may also appeal to people who want a non-pharmacological treatment option, a non-invasive next step before considering more intensive interventions, or a highly personalized alternative to standard, one-size-fits-all therapies.
Before starting treatment, patients complete a full consultation and clinical assessment. This usually includes:
This evaluation helps determine whether TMS is appropriate clinically and whether prior treatment history supports insurance authorization.
Some patients may not be candidates for TMS or may need additional evaluation first.
Examples include people with certain ferromagnetic metal implants near the head, cochlear implants, or specific implanted medical devices. A history of unprovoked seizures may require a case-by-case review. Pregnancy is also approached cautiously.
Even so, TMS generally has fewer barriers than more invasive interventions. It does not require anesthesia clearance, surgery, or hospitalization. A thorough consultation helps ensure treatment is both safe and appropriate. effects associated with deep brain stimulation or electroshock therapy
Treatment begins with a detailed evaluation.
During your first visit, the Neurotherapeutix team reviews your symptom history, previous medications, therapy experience, and treatment goals. OCD severity may be assessed using standardized tools such as Y-BOCS.
Functional imaging (fMRI) is at the heart of our targeted approach. We use this advanced technology to identify your specific brain circuits, ensuring every TMS session is precisely guided and personalized to your unique neurobiology.
A typical TMS course for OCD involves sessions five days per week for four to six weeks, with a total of about 20–40 sessions. Each session usually lasts about 20–30 minutes.
During treatment:
Because TMS is fully outpatient, many patients fit treatment into their workday or regular weekly routine.
Most patients tolerate TMS well. The most common side effects are mild scalp discomfort or a headache during the first few sessions, which often improve over time.
We closely monitor your progress throughout your treatment. This includes regular symptom reviews, ongoing severity assessments, and follow-up imaging to measure effectiveness and refine your personalized treatment plan as needed.
Some patients begin noticing changes within two to three weeks, while others experience more gradual improvement over the full course.
At the end of treatment, the team discusses next steps, which may include maintenance sessions, ongoing therapy, medication coordination, or continued monitoring. The results of your follow-up fMRI carefully guide these recommendations.
TMS is not presented as a cure, and it is important to set realistic expectations. The goal is meaningful symptom reduction and improved daily functioning. With our advanced fMRI-TMS technology, we deliver higher success rates, more significant symptom reduction, and long-lasting results.
For many patients, success looks like:
Some people respond early in treatment, while others notice the biggest changes closer to the end of the protocol.
For some patients, TMS results can last for months or longer.
Others benefit from maintenance sessions or booster treatments over time.
The ideal follow-up plan is uniquely tailored to each patient. It is guided by your post-treatment fMRI results, your symptom history, treatment response, and whether other therapies remain part of your ongoing care.
Exposure and response prevention, or ERP, remains the gold-standard psychotherapy for OCD.
TMS may work especially well as part of a comprehensive approach that includes ERP, medication management, or both.
In some cases, TMS may help reduce the symptom burden enough that ERP becomes more manageable.
While traditional TMS is often used alongside other treatments, the advanced precision and enhanced potency of our fMRI-guided TMS allow it to deliver profound results on its own.
SSRIs are often the first-line medication treatment for OCD. Common examples include fluoxetine, sertraline, fluvoxamine, and paroxetine. Clomipramine is also used in some cases.
While medications can help many people, they do not work well enough for everyone. Some patients experience only partial symptom relief, while others discontinue treatment due to side effects.
TMS may be considered after one or more medication trials have failed to provide adequate benefit. It can also be valuable for patients with overlapping depression or anxiety symptoms.
Exposure and response prevention is the most established psychotherapy for OCD. It helps people gradually face feared situations or thoughts without performing compulsions. ERP is highly effective, but it can also be difficult, especially when OCD-related anxiety is severe.
TMS may complement ERP by reducing the intensity of obsessive distress, making it easier for some patients to engage fully in treatment. Rather than replacing ERP, TMS can support a more comprehensive and integrated plan.
For severe and highly treatment-resistant OCD, more invasive interventions such as deep-brain stimulation may sometimes be discussed. DBS is a surgical procedure and is generally reserved for limited cases after multiple other treatments have failed.
ECT is not a standard first-line treatment for OCD and is more commonly used for severe depression. Because TMS is non-invasive and FDA-cleared specifically for OCD, it is often the preferred brain-based treatment to explore before more invasive options are considered.
Neurotherapeutix offers a more personalized approach to OCD treatment by combining FDA-cleared TMS technology with functional imaging-guided precision.
Patients choose Neurotherapeutix because we provide:
Our office on the Upper East Side offers convenient access for patients throughout New York City and beyond.
Treatment is structured to fit into daily life as much as possible, and our team works closely with each patient to create a plan that feels clear, supportive, and manageable.
Neurotherapeutix is a private-pay practice, allowing us to focus entirely on providing highly personalized, advanced care. While we are an out-of-network provider and do not interface directly with insurance companies or submit claims on your behalf, we support your efforts to seek reimbursement. Upon request, we will gladly provide you with your medical records, clinical progress notes, and an itemized billing statement (superbill) containing your procedure descriptions and billing codes, which you can use to submit a claim to your insurance plan.
It may be time to seek treatment if OCD is consuming more than an hour a day, interfering with work or relationships, causing you to avoid situations, or continuing despite medication or therapy.
OCD often becomes more disruptive when left untreated. Early and appropriate care can help reduce symptom severity and improve long-term functioning.
If your symptoms have not improved enough with standard treatment, or if medication side effects have made it difficult to continue, now may be the right time to explore another option.
You do not need to wait until symptoms become unbearable. Reaching out early can help you better understand what support is available.
Seeking treatment for OCD takes courage, especially if previous approaches have left you feeling discouraged. If you are exploring your next option, Neurotherapeutix is here to help you understand whether TMS may be a good fit.
When you contact our team, we can review your treatment history, explain the consultation process, and help you prepare for your first visit. This includes discussing prior medications, therapy history, and any previous assessments that may be helpful.
There is no pressure and no obligation. The goal is to provide clear information and compassionate guidance so you can make an informed decision about care.
If you are ready to move forward, you can contact our team directly or request an appointment online.
TMS received FDA clearance for the treatment of OCD in 2018, based on clinical research demonstrating safety and effectiveness.
At Neurotherapeutix, we use FDA-cleared TMS technology with computational brain mapping to provide more personalized treatment for obsessive-compulsive disorder in New York City.
A standard TMS course for OCD usually involves sessions five days a week for four to six weeks, for a total of about 20–40 sessions. Each session lasts about 20–30 minutes.
Many patients begin noticing improvement within 2 to 3 weeks, with continued progress throughout the full course.
TMS is generally well-tolerated and non-invasive. Most people feel a tapping sensation on the scalp during treatment rather than pain. No anesthesia is required, and there is no memory loss.
Mild scalp discomfort or headache can occur early in treatment, but these effects usually improve quickly.
Clinical studies suggest that about 40–50% of people with OCD may experience significant symptom improvement with TMS therapy.
At Neurotherapeutix, our functional imaging-guided (fMRI) targeting adds a crucial layer of personalization to your treatment plan. Compared to standard TMS, this precision approach delivers higher efficacy rates and yields longer-lasting relief.
It depends. Many insurance plans cover TMS for OCD when previous treatment has not provided enough relief. Coverage varies by insurer and plan.
As a private-pay practice, Neurotherapeutix does not directly handle insurance verification, prior authorization, or claims. However, to assist you in seeking out-of-network reimbursement, we provide your medical records, clinical notes, and detailed billing information, including procedure descriptions and codes.
Yes. Many patients continue taking their current medications during TMS therapy. TMS is often used alongside SSRIs or other psychiatric medications as part of a comprehensive treatment plan.
Any medication changes should be made only with your prescribing clinician’s guidance.lts of your follow-up fMRI carefully guide these recommendations.
Call us at (917) 388-3090 or click to request a regular or telehealth appointment.
Neurotherapeutix
171 East 74th Street, Unit 1-1 New York, NY 10021

Neurotherapeutix is the leading clinic for functional imaging guided transcranial magnetic stimulation (TMS), a safe, innovative, and non-invasive methodology for treating a wide range of acute and chronic mental disorders and brain injuries. Our advanced fMRI technology allows us to map the brain for the… Learn More »
By: Neurotherapeutix NYC
Reviewed By: Marta Moreno, Ph.D
Published: March 24, 2023
Last Reviewed: March 5, 2026
QUICK INQUIRY
Contact us to get an estimate for your medical services requirements. You can fill in the form to specify your medical requirements or you can call us directly.