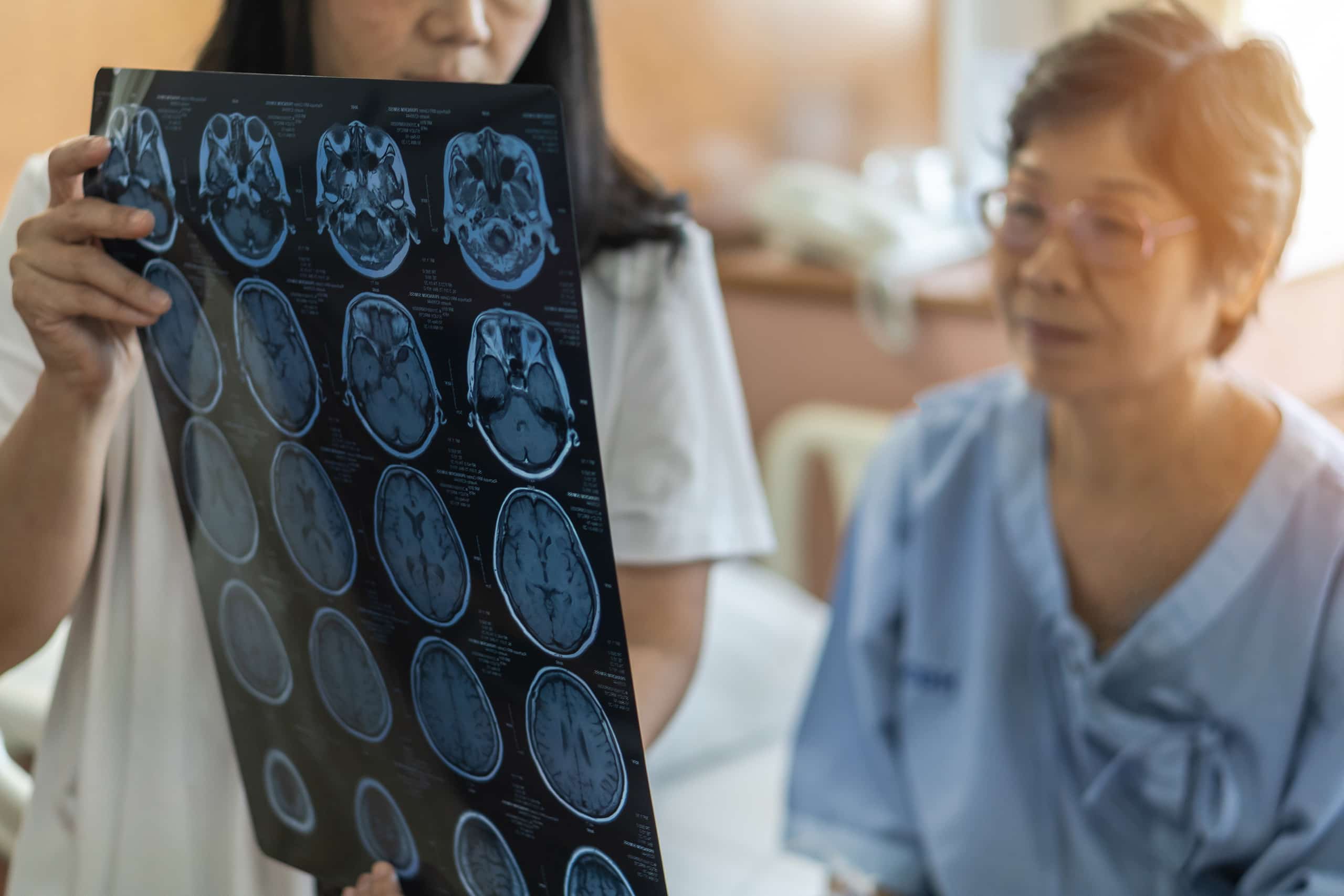
Functional neurological disorder (FND) can cause symptoms such as tremors, weakness, seizures, or difficulty speaking, even when standard brain scans appear normal. These symptoms are real and often disruptive, reflecting problems with how the brain communicates with the body rather than structural damage.
Because FND involves disruptions in brain signaling, researchers are exploring treatments that target these communication pathways directly. One emerging option is transcranial magnetic stimulation (TMS), a non-invasive therapy that uses magnetic pulses to influence activity in specific brain regions.
At Neurotherapeutix, clinicians use advanced fMRI-guided TMS to deliver highly personalized treatment, precisely targeting stimulation based on your individual brain activity and connectivity patterns. Understanding how TMS works may help people with FND explore new treatment possibilities.
What is functional neurological disorder (FND)?
Functional neurological disorder refers to a group of conditions in which the nervous system does not function properly, even though the brain’s physical structure appears normal.
The problem lies not in structural damage, but in how the brain sends and receives signals.
According to information from the National Institute of Neurological Disorders and Stroke (NINDS), FND can produce symptoms that closely resemble other neurological diseases. Yet, traditional imaging often fails to identify a clear structural cause.
Understanding the diagnosis
People living with FND may experience a wide range of neurological symptoms, including:
- Limb weakness or paralysis
- Tremors or abnormal movements
- Difficulty walking or balance problems
- Non-epileptic seizures (also called functional seizures)
- Speech or swallowing difficulties
- Sensory disturbances
- Cognitive fog or fatigue
Despite its prevalence, awareness of FND remains limited, which contributes to delayed diagnoses and limited access to specialized treatment.
Why FND is often misunderstood
Historically, conditions now classified as functional neurological disorders were sometimes labeled using outdated terms such as “conversion disorder” or “hysteria.” These labels often implied that symptoms were psychological or not medically legitimate.
Modern neuroscience has challenged these assumptions.
Today, clinicians understand that FND involves dysregulation in the brain’s functional networks. These networks coordinate movement, perception, emotional regulation, and cognition.
In people with FND, these communication pathways may become disrupted, leading to symptoms even though the brain’s structure appears intact.
Because FND sits at the intersection of neurology and psychiatry, our primary approach utilizes fMRI-guided TMS to precisely map and modulate the specific brain activity and connectivity patterns underlying the disorder, while also integrating multidisciplinary strategies to address contributing behavioral factors.
For many patients, recognizing that FND is a legitimate neurological condition is an important step toward recovery.
How the brain misfires in FND
To understand how treatments like TMS may help, it’s useful to understand what happens in the brain during functional neurological disorder.
The brain-body communication breakdown
The brain can be thought of as a complex communication network.
Under normal circumstances, signals travel from the brain through the spinal cord to muscles and sensory organs. These signals allow us to move, feel sensations, speak, and coordinate our actions.
In FND, these pathways remain intact, but the signals that traverse them may become disrupted or misdirected.
Researchers studying brain connectivity have identified differences in several key brain regions in people with FND, including:
- Motor planning areas
- The prefrontal cortex
- The limbic system, which regulates emotions
- Sensory processing regions
Functional MRI studies suggest that these networks may become dysregulated, leading to symptoms even when the underlying brain structure remains intact.
The role of neuroplasticity
One important concept in neuroscience is neuroplasticity, the brain’s ability to change and reorganize itself.
Neuroplasticity is what allows your brain to learn new skills, adapt to new experiences, and even recover from injury. But this same adaptability can also work against you. When abnormal signaling takes root, the brain can effectively “learn” and reinforce these dysfunctional, maladaptive pathways over time.
The encouraging news? If the brain can learn these negative patterns, it also has the power to unlearn them.
That is where our advanced neuromodulation therapies come in. By utilizing fMRI-guided TMS, we can precisely target and interrupt these locked-in pathways, encouraging your brain to actively relearn healthier, more optimal communication patterns.
What is TMS, and how does it work?
Transcranial magnetic stimulation (TMS) is a non-invasive, precision-based therapy that utilizes magnetic pulses to physically reshape and improve activity and connectivity patterns in targeted regions of your brain.
The science behind transcranial magnetic stimulation
During TMS treatment, a coil is placed gently against the scalp. This coil generates brief magnetic pulses that pass through the skull and stimulate neurons in specific brain areas.
These magnetic pulses induce small electrical currents in the targeted neurons. Over time, repeated stimulation can alter how brain networks communicate.
TMS has been extensively studied and is currently FDA-cleared for the treatment of major depressive disorder and obsessive-compulsive disorder. Millions of treatment sessions have been delivered worldwide.
TMS is generally well-tolerated and does not require anesthesia. Most people remain awake and alert during treatment and can resume normal activities afterward.
Different types of TMS
Not all TMS treatments are the same.
Traditional TMS protocols often rely on standardized targeting based on general anatomical landmarks. While this approach has been effective for some conditions, it may not fully capture the unique brain network patterns present in each individual.
At Neurotherapeutix, clinicians use fMRI-guided TMS therapy, which combines neuromodulation with advanced brain imaging.
Utilizing advanced computational brain mapping, our expert clinicians can precisely identify abnormal activity and map out exactly where vital communication across your brain networks has been disrupted.
This precise imaging data allows our physicians to design a fully customized stimulation protocol, targeting the exact neural pathways responsible for your individual symptoms.
Unlike standardized, “one-size-fits-all” approaches, this method allows our clinicians to deliver stimulation precisely to the areas of your brain where communication breakdown is actually occurring.
The evidence: Can TMS help functional neurological disorder?
Research into TMS for FND is still developing, but early findings suggest that neuromodulation may help restore communication within brain networks involved in functional symptoms.
What the research shows
Several studies have explored the potential of TMS for treating functional neurological disorders.
A study published by Nicholson and colleagues in 2016 reported early evidence that TMS may help improve symptoms in some individuals with functional movement disorders.
More recently, a review published in Brain Stimulation (Gonsalvez et al., 2021) examined emerging evidence for neurostimulation techniques in FND. The authors concluded that neuromodulation therapies such as TMS show promise as part of a broader treatment strategy for functional neurological symptoms.
Researchers believe TMS may help by:
- Restoring communication between disrupted brain networks
- Encouraging neuroplastic changes that support healthier signaling patterns
- Modulating overactive or underactive regions involved in symptom generation
While large-scale clinical trials are still ongoing, early findings suggest that targeted brain stimulation may help reduce symptom severity in some patients.
What to expect: The TMS treatment process for FND
Understanding the treatment process can help patients feel more comfortable when considering TMS therapy.
Initial evaluation and computational brain mapping
Treatment typically begins with a comprehensive clinical evaluation.
At Neurotherapeutix, this comprehensive evaluation may include resting-state functional MRI brain mapping, allowing our clinicians to precisely measure both the unique activity levels and the complex connectivity patterns across your brain’s networks.
The process is simple: patients lie comfortably in an MRI scanner while their brain activity is gently recorded. The resulting data allows our physicians to identify precisely where communication between brain regions has been disrupted, and we use this critical information to design a fully personalized stimulation protocol.
The fMRI-guided TMS sessions
A typical TMS course involves 20–40 sessions delivered over four to six weeks. For patients seeking faster results, we also offer accelerated protocols where multiple sessions are completed each day over consecutive days.
Each session usually lasts between 20 and 40 minutes.
During treatment, patients may feel a tapping sensation on the scalp where the magnetic coil is positioned. Some individuals experience mild scalp discomfort or temporary headaches, but serious side effects are rare.
No anesthesia or recovery time is required, and most patients resume normal activities immediately after treatment.
Monitoring progress
Throughout your treatment, our clinicians actively monitor your symptom changes, allowing us to adjust stimulation parameters and refine targeted brain locations as needed to ensure optimal results.
To take this monitoring a step further, we can also utilize follow-up brain imaging sessions. This advanced approach allows us to directly visualize and assess the positive changes occurring within your brain’s connectivity patterns as your therapy progresses.
While fMRI-guided TMS is highly effective as an independent therapy, patients can experience synergistic benefits when they combine their treatment with supportive care, such as psychotherapy, physical rehabilitation, or stress management.
Is TMS right for your FND?
TMS is a highly effective treatment option for individuals seeking advanced care for Functional Neurological Disorder. You may be a great candidate if you:
- Have a diagnosis of FND
- Have not found relief through conventional treatments
- Can participate in a structured treatment schedule
- Are medically cleared for TMS therapy
Our clinical team will work with you to review your neurological and psychiatric history, ensuring that TMS is a safe and highly targeted solution for your specific needs.
Questions to ask your doctor
If you are considering TMS for FND, it may be helpful to ask your doctor questions such as:
- How might imaging-based computational brain mapping help identify my symptom patterns?
- What does current research suggest about TMS for my type of symptoms?
- How will we measure whether treatment is working?
- What other therapies should be used alongside TMS?
- What timeline should I expect for improvement?
These discussions can help patients make informed decisions about their care.
Taking the next step with Neurotherapeutix in New York City
FND affects how the brain communicates with the body, often causing significant symptoms despite normal structural scans.
Powerful new therapies like TMS are changing the landscape of FND treatment by restoring healthy brain communication. At Neurotherapeutix, we take this a step further: our fMRI-guided TMS utilizes advanced brain imaging to map your specific neural networks, allowing us to deliver a completely personalized, highly targeted stimulation treatment designed just for you.
If you’re looking for a more effective approach to FND, request an appointment to learn how our experts can design an fMRI-guided TMS treatment plan tailored completely to your unique healing journey.
Frequently asked questions about TMS for FND
Is TMS FDA-approved for FND?
TMS is currently FDA-cleared for conditions such as depression and obsessive-compulsive disorder. Its use for FND is considered off-label, meaning physicians may recommend it based on clinical judgment and emerging research evidence.
Does insurance cover TMS for FND?
Insurance coverage varies widely depending on the diagnosis and treatment protocol. Some insurance plans cover FDA-cleared TMS treatment for depression, but coverage for FND may be more limited.
Patients should contact their insurance provider to verify coverage.
Is TMS painful or dangerous?
TMS is generally well tolerated. Most people experience only mild scalp sensations during treatment.
Serious side effects are rare, and millions of TMS sessions have been delivered safely worldwide.
How long does it take to see results?
Some patients begin noticing changes within two to three weeks, while others may see improvement later in the treatment course.
Because responses vary, clinicians monitor symptoms closely throughout therapy.
How effective is TMS for FND?
While standard TMS helps reduce FND symptoms by stimulating the brain, our advanced fMRI-guided TMS takes your healing to the next level. By utilizing highly detailed functional imaging to map your brain’s specific activity and connectivity patterns, we eliminate the guesswork. This allows us to deliver personalized, pinpoint stimulation exactly to the neural networks that need it most. This unmatched precision drives superior, lasting outcomes—providing deeper symptom relief and empowering you to take back control of your life.