If you’re exploring transcranial magnetic stimulation (TMS) therapy, it’s natural to wonder whether Does insurance cover TMS? A complete NYC coverage guide
If you’re exploring transcranial magnetic stimulation (TMS) therapy, it’s natural to wonder whether insurance will help cover the cost.
Insurance coverage for TMS can be complex and depends on various factors.
In some cases, insurance may cover TMS therapy. Coverage decisions are typically made on a case-by-case basis and guided by insurer-specific criteria, and approval is never guaranteed.
Understanding how these decisions are made can help you feel more prepared as you explore treatment options for psychiatric conditions, neurodevelopmental disorders, or neurological diseases.
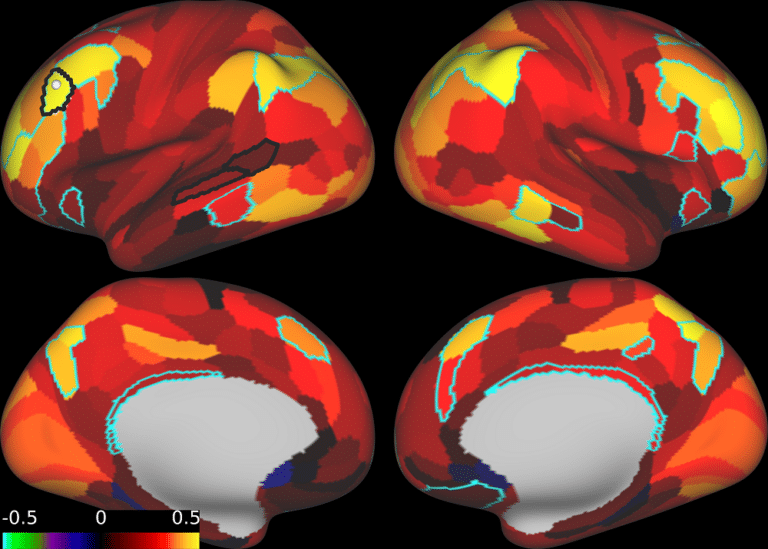
At Neurotherapeutix in New York City, treatment is delivered using fMRI-guided TMS therapy. This advanced approach uses functional brain imaging and computational brain mapping to personalize stimulation targets for each patient. If you would like to learn more about fMRI-guided TMS, you can explore how this personalized, precision-based therapy works and how it differs from standard TMS protocols.
This guide explains how insurance coverage for TMS therapy is typically evaluated, what factors influence approval, and what options may be available if insurance does not cover treatment.
How TMS insurance coverage works
Insurance providers rely on defined clinical criteria when evaluating whether TMS qualifies for coverage. These criteria vary by insurer and plan.
In most cases, insurers evaluate several factors before deciding whether a treatment will be reimbursed. These often include diagnosis, medical necessity, treatment history, and the specific treatment protocol being recommended.
Because policies vary widely, coverage decisions are made by the insurance provider rather than the treating clinic.
Understanding how insurers evaluate these factors can help patients better navigate the insurance verification process.
When insurance may cover TMS therapy
Insurance providers rely on defined clinical criteria when evaluating whether TMS qualifies for coverage.
Medical necessity and diagnosis requirements
When insurance coverage is approved, it is typically tied to documentation showing that TMS is medically necessary for a specific condition.
One commonly cited example in insurance policies is major depressive disorder (MDD), particularly when symptoms are persistent or severe.
However, TMS therapy is being studied and used for a broader range of conditions affecting brain function. These may include:
Psychiatric conditions
- Anxiety disorders
- Obsessive-compulsive disorder (OCD)
- Post-traumatic stress disorder (PTSD)
- Bipolar disorder
Neurodevelopmental disorders
- Autism spectrum disorder
- Asperger’s syndrome
- ADHD
- Learning disabilities
- Tourette syndrome
Neurological diseases and brain injuries
- Parkinson’s disease
- Traumatic brain injury (TBI)
- Stroke recovery
- Migraine disorders
- Cognitive decline
While TMS therapy may be considered for a wide range of brain-based conditions, insurance coverage policies are typically narrower and often focus on major depressive disorder.
Coverage guidelines differ widely. Some insurance plans are narrowly defined, while others allow broader interpretation based on clinical documentation and medical review.
Prior treatment history and step therapy
Insurance approval for TMS often depends on prior treatment history. This may include documentation showing that other standard treatments did not provide sufficient symptom improvement or were not well tolerated.
This requirement is often called step therapy, which means patients must first try more conventional treatments before advanced therapies are considered.
Examples of prior treatments insurers may require include:
- Antidepressant medications
- Mood stabilizers or psychiatric medications
- Psychotherapy or counseling
- Combination treatment approaches
The number and type of treatments required before TMS therapy can vary significantly between insurance providers.
Because each insurance company uses its own review process, approval requirements may differ even between plans offered by the same insurer.
Common insurance providers and TMS coverage
Coverage policies vary by insurance plan and provider.
Private insurance
Some private insurance plans may cover standard TMS therapy when specific diagnostic and treatment history requirements are met.
Insurance companies that sometimes provide coverage for TMS therapy include:
- Aetna
- Blue Cross Blue Shield
- UnitedHealthcare
- Cigna
- Oxford Health Plans
Prior authorization is typically required before treatment begins. Approval depends on how closely the proposed treatment aligns with the insurer’s established coverage criteria.
Even within the same company, coverage policies may vary between individual plans.
Medicare and Medicaid
Medicare may cover TMS therapy under certain circumstances when medical necessity requirements are met.
Coverage is often considered for patients diagnosed with treatment-resistant depression, meaning symptoms have not improved after multiple medication trials.
Medicaid coverage varies by state and is often more limited.
In New York, Medicaid policies may allow TMS coverage in certain situations, but specific requirements vary by plan and provider network.
Because insurance policies change over time, it is always important to verify coverage details directly with your insurance provider.
Why coverage varies by clinic and technology
Insurance coverage for TMS is influenced not only by diagnosis but also by how treatment is delivered.
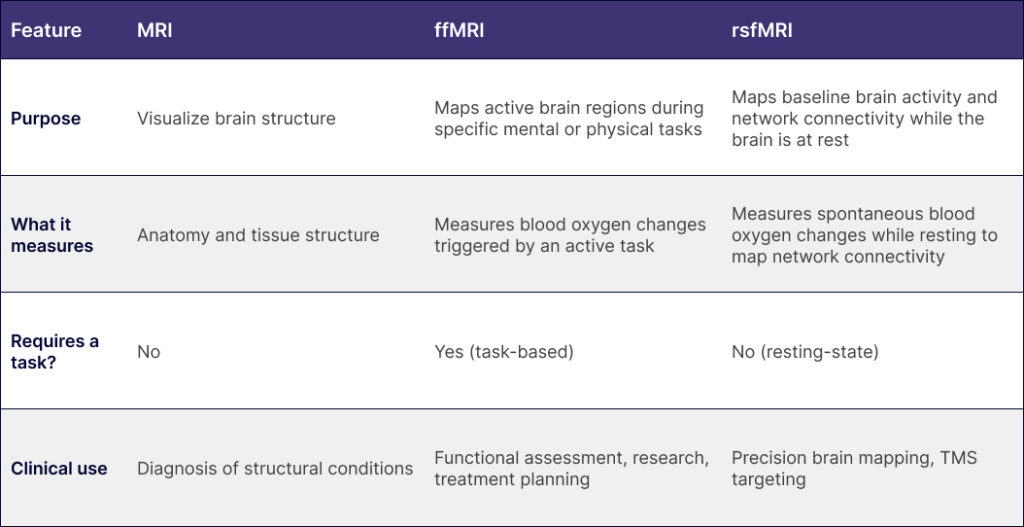
Standard vs. advanced fMRI-guided TMS therapy
Most insurance policies are built around standard TMS protocols, which rely on generalized stimulation targets based on anatomical landmarks rather than each patient’s unique brain activity and connectivity patterns.
These standardized approaches are easier for insurers to evaluate because they follow fixed treatment protocols.
At Neurotherapeutix, treatment is delivered using fMRI-guided TMS therapy, informed by functional MRI–based computational brain mapping.
This approach allows clinicians to tailor stimulation targets to each individual’s unique brain activity and connectivity patterns. By identifying how specific brain networks function, treatment can be personalized to focus on the neurological pathways underlying a patient’s condition.
Because fMRI-guided TMS therapy represents an advanced, precision-based methodology, it is not typically included within standard insurance reimbursement frameworks.
As a result, coverage decisions may vary based on treatment technology and clinical approach rather than solely on patient need.
Insurance requirements for TMS therapy
When insurance companies evaluate TMS therapy coverage, they often consider several key criteria.
Diagnosis documentation
Most insurers require documentation confirming a qualifying diagnosis. For many policies, this diagnosis is major depressive disorder.
Treatment-resistant symptoms
Insurance providers may require documentation showing that symptoms have not improved after previous treatment attempts.
This may include records of medication trials or psychotherapy that did not produce adequate symptom relief.
Prior authorization
Many insurance companies require prior authorization before TMS therapy can begin.
This means the insurer reviews clinical documentation to determine whether the treatment meets its coverage criteria.
Treatment protocol requirements
Some insurance providers also specify details regarding how TMS therapy must be delivered, including the number of sessions or treatment schedule.
Because requirements vary between insurers, it is important to confirm the details of your individual plan.
What if TMS therapy isn’t covered by insurance?
If insurance does not cover TMS therapy, there may still be options to consider.
Out-of-network reimbursement
Some patients choose to pursue treatment and submit claims independently to their insurance provider for possible reimbursement.
In these cases, patients pay for treatment upfront and then submit documentation for reimbursement consideration.
Reimbursement decisions vary by plan and are not guaranteed.
Paying out of pocket
When insurance coverage is not available, fMRI-guided TMS therapy at Neurotherapeutix is offered as a self-pay service.
This allows treatment decisions to be guided by clinical goals rather than insurance restrictions.
Patients can discuss financial considerations with our care team to evaluate options thoughtfully and without pressure.
How Neurotherapeutix helps patients navigate insurance questions
Navigating insurance decisions can feel overwhelming, especially when you’re already focused on your health or supporting a loved one.
At Neurotherapeutix, we help patients:
- Understand in general terms, how insurance plans may view TMS coverage
- Clarify why coverage can differ across clinics and treatment technologies
- Explore treatment costs and payment options transparently
- Receive clear documentation and billing details to support any insurance reimbursement you choose to pursue independently
Neurotherapeutix is a private-pay practice. We do not submit information to insurance, call insurance companies, or handle insurance claims on behalf of patients. Instead, we provide medical records, reports, and billing codes so that patients who wish to seek reimbursement can submit claims directly to their own insurance plans.
Exploring next steps with confidence
Insurance coverage is only one part of the decision-making process when considering TMS therapy.
For many patients, clearly understanding their options and feeling supported throughout the process are just as important as reimbursement decisions.
Neurotherapeutix provides advanced fMRI-guided TMS therapy designed to support brain health across a wide range of psychiatric, developmental, and neurological conditions.
Patients who want to learn more about treatment can also hear from patients who’ve experienced results, review frequently asked questions about TMS, or speak with specialists about personalized treatment recommendations.
If you are exploring treatment options, you can explore patient stories, review our frequently asked questions and answers, contact us directly, or request an appointment to discuss your situation and learn whether TMS therapy may be appropriate for you.
Frequently asked questions about TMS insurance coverage
Is TMS therapy usually covered by insurance?
Sometimes. Coverage depends on diagnosis, treatment history, insurance provider, and how the therapy is delivered. Approval is not guaranteed.
Does Medicare cover TMS therapy?
Medicare may provide coverage for TMS therapy under specific circumstances when medical necessity criteria are met. Coverage details vary and should be confirmed directly with Medicare.
Will insurance cover fMRI-guided TMS?
Most insurance policies are written in accordance with standard TMS protocols. Advanced imaging-guided approaches are not typically included in traditional insurance reimbursement frameworks.
What if my insurance denies TMS treatment?
If coverage is denied, you may still explore options such as out-of-network reimbursement or self-pay treatment. Your provider can help explain potential next steps.
Can I get reimbursed if I pay out of pocket for TMS?
Some insurance plans allow patients to submit claims independently for possible reimbursement. Approval depends on individual plan benefits and is not guaranteed.